This feature is part of our Paramedic Chief Digital Edition, a regular supplement to EMS1.com that brings a sharpened focus to some of the most challenging topics facing paramedic chiefs and EMS leaders everywhere. To read all of the articles included in the issue, click here.
Women who are or have been pregnant are very familiar with the quick, non-invasive and painless capability of ultrasound.
But what about the EMS provider in the back of a rig with a cardiac arrest patient en route to a hospital?
There are many tools at providers’ disposal when it comes to patient care and assessment, but point-of-care ultrasound can take patient treatment to the next level.
And while some argue that agencies should be paring down equipment placed on ambulances rather than adding diagnostic tools, others couldn’t disagree more.
Jason Bowman, a fourth-year medical student planning a career in emergency medicine and critical care and a member of EMSPOCUS, has a different philosophy and mindset when it comes to using ultrasound in the field.
Hocus POCUS
Bowman got his start in medicine as a volunteer firefighter/EMT in 2004. He worked for several different EMS agencies, from county to hospital to fire-based. Eventually, he worked his way up to critical care paramedic and was a medic instructor for a few years. He has been dubbed a “bonafide ultrasound nerd” by his colleagues – a nickname he’s quite proud of.
“Since 2009, I’ve carried an ultrasound machine with me, either in my bag or in my truck,” Bowman said. “I’ll show it off to anyone who will listen.”
Point-of-care ultrasound, the use of ultrasound to answer simple yes/no clinical questions at the patient’s bedside, differs from comprehensive ultrasounds that sonographers perform. Ultrasound, according to Bowman, may be classified as an imaging modality, but it’s not like a photograph or X-ray.
“To do the ultrasound, you have to touch your patient. It’s like having X-ray vision during your physical exam,” he said. “It becomes an extension of your eyes and hands and lets you peer under their skin to see exactly what’s going on. And when you clinch that surprise diagnosis and completely change a patient’s care, there’s nothing else like it.”
Bowman also stated that point-of-care ultrasound is more versatile than 12-lead EKGs and can be performed in roughly the same amount of time.
“We can truly diagnose people in the field – something we can rarely do without imaging,” he said.
Bowman’s philosophy is to make sure to train the providers using point-of-care ultrasound to the max so that when you put an additional piece of equipment on a rig it gets used as often as possible.
Functional components of ultrasound
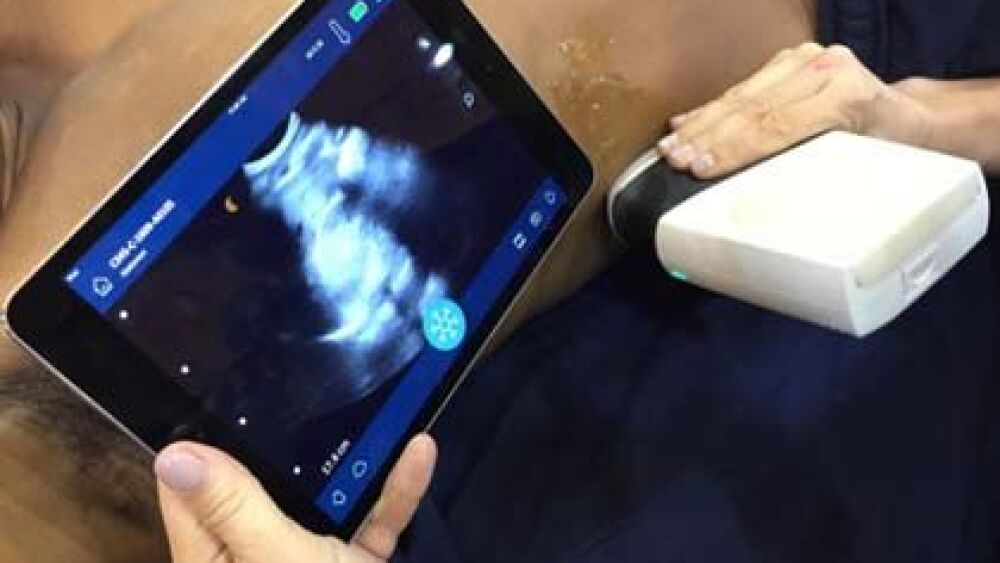
From the first enormous and hefty ultrasound scanners, circa 1965, to today’s pocket-sized and portable scanners, EMS providers now have more information at their fingertips – literally. Several manufacturers even make portable ultrasound systems that link to cellphones or tablets.
Although systems vary, all ultrasound tools have a screen to display the image and a probe to obtain it. There are multiple types of probes. While there’s some overlap, they’re not completely interchangeable.
“For most uses, I recommend having at least a linear and phased array probe for EMS, but curved arrays are nice to have if you can afford it,” Bowman said.
More basic are the necessary accessories. Ultrasound systems hate air; providers will need gel on hand to keep the probe in fluid contact with the patient.
And new uses for ultrasound keep getting added every year. Ten years ago, lung ultrasound was thought impossible by most. Now, it’s an EMS provider’s most useful exam.
“I think the actual scope of point-of-care ultrasound is far from filled out,” Bowman said. “This tool will only get more useful as time goes on.”
Prehospital uses for ultrasound
The most commonly performed exam, Bowman says, is the FAST exam looking for free fluid in trauma patients. But he said he doesn’t see a lot of utility in performing this type of exam.
“It takes about 500 milliliters of free fluid to leak into your abdomen before you can see it, and people that bleed that much in the 15 minutes it takes an ambulance to get there rarely look stable without ultrasound,” he said.
The same exam can also be used to diagnose a ruptured ectopic pregnancy. And ultrasound can detect pneumothorax, fluid overload, heart failure, sepsis, pulmonary embolism, PEA versus hypotension in cardiac arrest, assist with difficult IVs and even spot a middle cerebral artery stroke.
“We’ve had cardiac arrests that we were able to determine their rhythm without stopping chest compressions,” Bowman said. “We’ve diagnosed massive pleural effusions causing cardiorespiratory failure. And the field has changed significantly since then. There are multiple new exams that are considered mainstream that weren’t even around in 2010.”
There are, however, both benefits and drawbacks of using ultrasound to assess, treat and monitor patients.
Daniel Theodoro, MD, emergency medicine ultrasound section director at Washington University School of Medicine in St. Louis, said providers using point-of-care ultrasound can make a diagnosis of life-threatening emergencies in a matter of seconds.
“Conditions that cause death, if not recognized and treated within minutes, can be promptly addressed with point-of-care ultrasound,” Theodoro said, “for example, peritoneal hemorrhage in cases of trauma and abdominal aortic aneurysms and cardiac tamponade. It even helps in cases of septic shock, since we can quickly assess heart and fluid status and choose the right resuscitation strategy.”
For most, the biggest drawback is the cost. Indisputably, ultrasound isn’t cheap, and the proper training is hard to come by.
“The indications for point-of-care ultrasound haven’t been laid out yet – even for emergency physicians – so designing a ‘one size fits all’ curriculum is currently impossible,” Bowman said.
On the physician side, Theodoro said the biggest hurdle to using point-of-care ultrasound is the educational component.
“It usually takes 15 to 20 years before physicians start implementing advances in their everyday practice,” he said. “So when you run into a seasoned physician who wasn’t exposed to emergency medicine ultrasound training, they sometimes ask out loud why they should learn something new when they’ve been doing just fine without it.”
But while there’s more than one way to solve medical emergencies, Theodoro said he believes that point-of-care ultrasound is the best way.
“Point-of-care ultrasound represents new knowledge that must be absorbed, and that’s a challenge for new and seasoned physicians,” he said. “It can make any doctor the smartest doctor in the room once you know just how powerful of a tool it can be.”
Bowman said his crews often knew more about ultrasound than the ED doctors during patient transfer.
“Fortunately, the doctors tended to still be very receptive, and inviting them to your training classes to get free ultrasound training is a great way to make strong allies in the ER,” he said.
Real-world example
One of Bowman’s most surprising cases was a call for abdominal pain in an 18-year-old female. When crews arrived, they found that the woman was 28 weeks pregnant and in active labor.
“It’s rush hour and we are a good 45 minutes from the high-risk OB center and about 15 minutes from the local hospital,” Bowman said. “Anything past 23 weeks is potentially viable. The question in our mind was if this was a preterm labor or a miscarriage.”
Without ultrasound, most providers would have called a helicopter to get the patient to the high-risk center as soon as possible. Fortunately, Bowman’s crew had ultrasound on board. They had learned how to check fetal heart rates with ultrasound, but checking for fetal demise wasn’t part of the training.
“We pulled out the ultrasound, and immediately we could see the heart was not beating,” Bowman said. “A second paramedic performed the exam to confirm and agree – no fetal heartbeat. We called medical control with our findings and were told to treat for pain and take her to the local hospital. This case was a completely unexpected use of ultrasound that drastically changed her care.”
Theodoro’s “patient zero” was a 60-year-old female also complaining of abdominal pain. She was hypotensive, and he thought she was septic from an infection.
“I did a point-of-care ultrasound within five minutes of her arrival and found an 8-centimeteraortic aneurysm,” he said. “I called in our vascular surgeon, showed him our findings, and he said ‘let’s go’ and repaired her.”
What happened next, however, is what made Theodoro a believer in point-of-care ultrasound.
“The surgeon came down, after he had repaired her and saved her life, to give me a high five and said, ‘Thank goodness you did that, because she was starting to rupture just as we began our repair.’ I rarely do things that have that kind of impact. Point-of-care ultrasound gives you that power.”
Keeping interest high
Bowman’s mission is proving the powerful and positive impact on patient outcomes.
As a result, he started an ultrasound program at the fire department where he was working, sparked by a research project he needed to complete as part of his bachelor’s degree in emergency health sciences.
Bowman met Dave Spear, an ED doctor and former paramedic that started the first EMS ultrasound program in Odessa, Texas, at an EMS conference. Spear took Bowman under his wing and gave him an old ultrasound machine to use in the field.
Bowman trained his colleagues and got the program up and running, but things started going downhill.
“The chiefs were never really interested in doing ultrasound,” he said. “It sort of became ‘my’ thing and was no longer a ‘department’ thing. A lot of the guys stopped doing ultrasounds once they got the impression that it wasn’t going to stick around.”
Not long after, Bowman left the department to go to medical school. The chiefs had him pack up the machines and send them back.
“We’ve seen a lot of services start doing point-of-care ultrasound and then stop,” he said.
Bowman and Theodoro said the lack of support may have to do with the futility of the FAST exam.
“Nobody likes to do something that they don’t think is changing patient care,” Bowman said.
Theodoro and a small group of physicians trained in emergency medicine meet biweekly to review ultrasounds that were performed in the ED.
“Our group is committed to doing more advanced imaging techniques, such as evaluation of deep venous thrombosis, advanced cardiac imaging to determine cardiac function, lung ultrasound, ocular ultrasound and more,” Theodoro said.
Aware of the roadblocks, both in EMS and in hospitals, Bowman and Theodoro agree that point-of-care ultrasound unifies the concept of medicine and taking care of patients.
“I think any reasonable paramedic will see that what you get out of it is totally worth it,” Bowman said.
This article was originally posted on July 17, 2017. It has been updated.