This is the last article in a three-part series. First we looked at why we obtain a 12-lead EKG with the first set of vital signs and then we looked at why we perform serial 12-lead EKGs. Now we’re going to address an even more fundamental question.
Who should receive a 12-lead EKG in the first place?
The primary purpose of the 12-lead EKG is to screen patients for cardiac ischemia, especially for acute ST-elevation myocardial infarction. This allows EMS personnel to triage suspected acute STEMI patients to the most appropriate hospital (not necessarily the closest hospital) and it should allow prehospital activation of the cardiac cath lab which is particularly important on nights, weekends and holidays when the cath team needs to be called in from home.
How do we catch as many acute STEMIs as possible?
To answer this question we need to know how STEMI patients present. According to most studies approximately 80 percent of STEMI patients will present with a chief complaint of chest pain. Of course, that means that 20 percent (one out of five) will not present with classical chest pain (the so-called anginal equivalents).
That’s why we need to cast as wide a net as possible (within reason) we screen patients with possible acute coronary syndrome.
What are the indications for a 12-lead EKG?
My department has a protocol that specifically deals with who should receive a 12-lead EKG. The indications include:
- Chest pain
- Atypical chest pain
- Epigastric pain
- Back, neck, jaw or arm pain without chest pain
- Palpitations
- Syncope or near syncope
- Pulmonary edema
- Exertional dyspnea
- Weakness
- Diaphoresis unexplained by ambient temperature
- Feel of anxiety or impending doom
- Suspected diabetic ketoacidosis
Note: Many protocols also include altered mental status although these patients should receive a CT scan prior to being sent to the cardiac cath lab. Neurological insult can sometimes cause ST/T-wave changes that mimic acute STEMI.
It’s well understood that the vast majority of these patients will not be experiencing an acute STEMI, but that’s okay! Tim Phalen sometimes compares performing a prehospital 12-lead EKG to “panning for gold.” The bottom line is that we can’t tell who is experiencing an acute STEMI by just looking at them. That’s not to say the physical exam isn’t important - it is. But it’s the 12-lead EKG that should trigger the reperfusion process in an effective STEMI system.
I’ve heard many times that experienced paramedics don’t need a 12-lead EKG to identify a heart attack patient, or that experienced paramedics can tell when chest pain is “non-cardiac” or symptoms can be attributed to some other process. I would argue that experience can teach us when acute STEMI is less likely, but we should still perform a 12-lead EKG.
Case: Patient dehydrated while kayaking
EMS responded to a patient who had been out kayaking on a hot and humid day. He started to feel dehydrated, became weak and nauseated, and vomited. He looked ill so bystanders called 9-1-1. By the time paramedics arrived at the patient’s side the bystanders had given him water and the patient was feeling better.
Paramedics placed him on the cardiac monitor as part of their evaluation. No 12-lead EKG was performed. After all, it was obvious why this patient was dehydrated. He had been out kayaking on a hot and humid day.
Fortunately, the patient consented to being transported to the hospital.
Here is the 12-lead EKG that was obtained on arrival in the emergency department.
As it turned out the cardiologist was attending another patient in the emergency department when the Code STEMI was called and the patient had an excellent door-to-balloon time.
Before
After
This story had a happy ending, but the patient dodged a bullet, and that’s not good from a patient safety perspective.
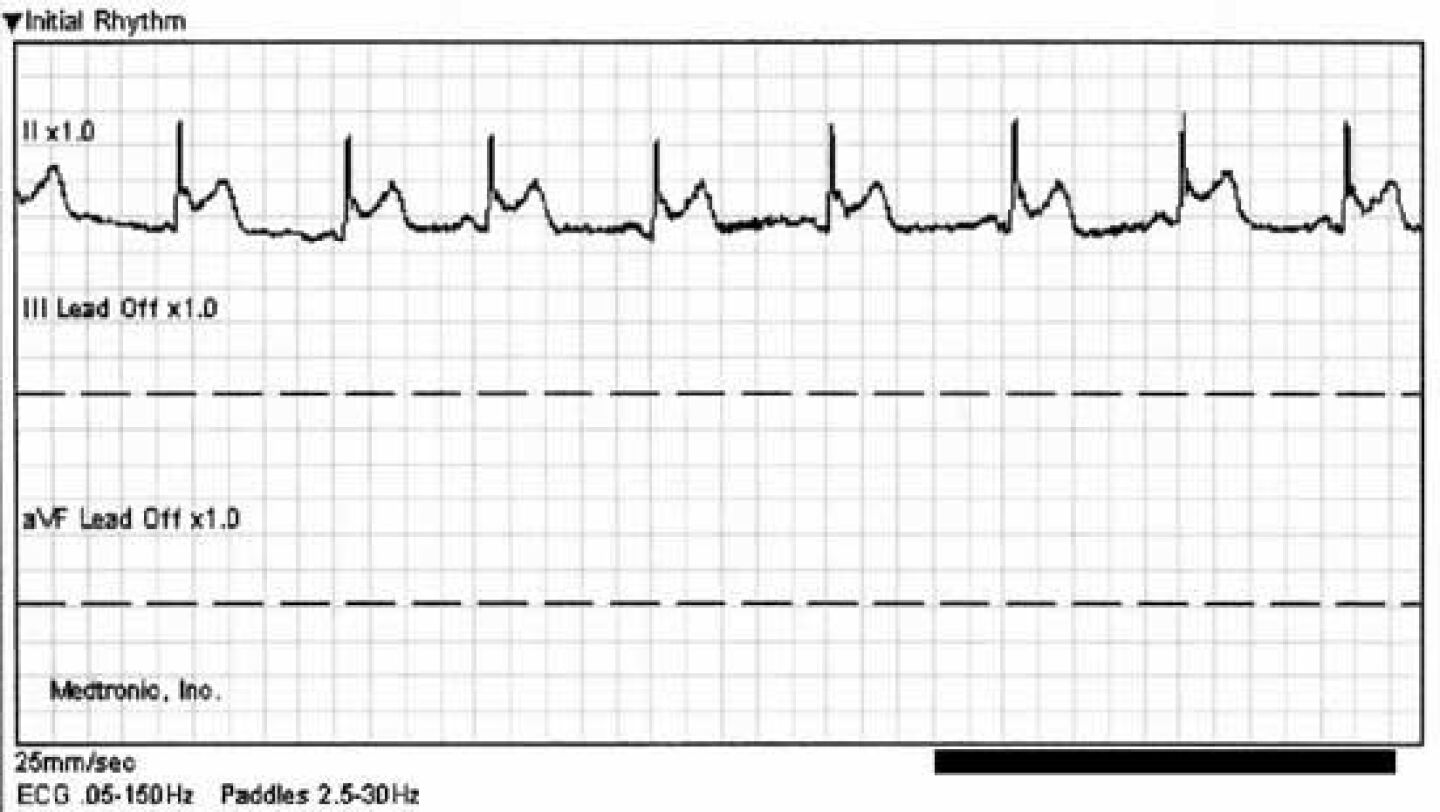
I’m sure that many of you picked up on the ST/T-wave abnormality in the 3-lead EKG and believe that would have triggered you to perform a full 12-lead EKG. While that may be true, I think it’s particularly unwise to screen patients with a 3-lead EKG unless you’re only interested in their heart rhythm.
For one thing, when you’re in “monitor mode” the low-frequency/high-pass filter is typically set to 1 Hz and will not display ST-segments accurately. To fully appreciate this point let’s show the exact some rhythm strip in “diagnostic mode” with the low frequency/high pass filter set to 0.05 Hz.
In addition, there are certain types of LAD occlusions that show nothing but ST-elevation in the precordial leads! That means you won’t even see reciprocal changes in the limb leads. You simply cannot do an adequate job screening patients for cardiac ischemia with a 3-lead EKG in monitor mode.
Some EMS systems have had such a hard time with paramedics delaying the 12-lead EKG because the patient is “already on the monitor” that they’ve insisted that the monitor not be powered on until all 10 electrodes are attached. That may sound extreme but this particular EMS system has one of the best “arrival on scene to 12-lead EKG” times in the business. In other words, the rule achieved the desired result.