Light yellow, mild aroma, minimal foam and slightly salty to taste.
It may sound like a new microbrew, but we’re actually talking about urine. This concoction is prepared in your kidneys through miles of microscopic tubing with strategically placed channels and cellular pumps. The kidney’s mission is to maintain the right balance of water, salts (sodium, chloride, potassium, etc.) and acids to sustain life. This balancing act is dependent on feedback from various body sensors (pituitary gland, adrenal glands) that produce traveling signals (hormones like antidiuretic hormone and aldosterone) that direct the kidneys to excrete more or less water, salts and acids.
Remember water follows sodium, so the key to water balance is the excretion or reabsorption of sodium by the kidneys. Water also follows other molecules that can be abnormally excreted in overabundance, such as glucose in the hyperglycemic patient — which explains why they are often dehydrated.
The kidneys excrete urea, the waste byproduct of protein breakdown, and they also produce erythropoietin, a hormone that stimulates the bone marrow to produce red blood cells. This hormone can also be administered as an injection for patients who are low on red blood cells (anemia) when the cause of the anemia is due to inadequate production of this substance, often caused by kidney failure.
What are symptoms of dehydration?
Symptoms of dehydration can range from mild to severe and may include:
- Dry mouth,
- Dark yellow urine,
- Dizziness
- Fatigue
- Decreased urine output
Generally, we take in more water and salt than we need, thus most of the time, the kidneys are busy excreting excess water and salt in order to maintain a balance. However, there are times when we experience inadequate ingestion of salt and water, or excessive loss of salt and water, or a combination of both.
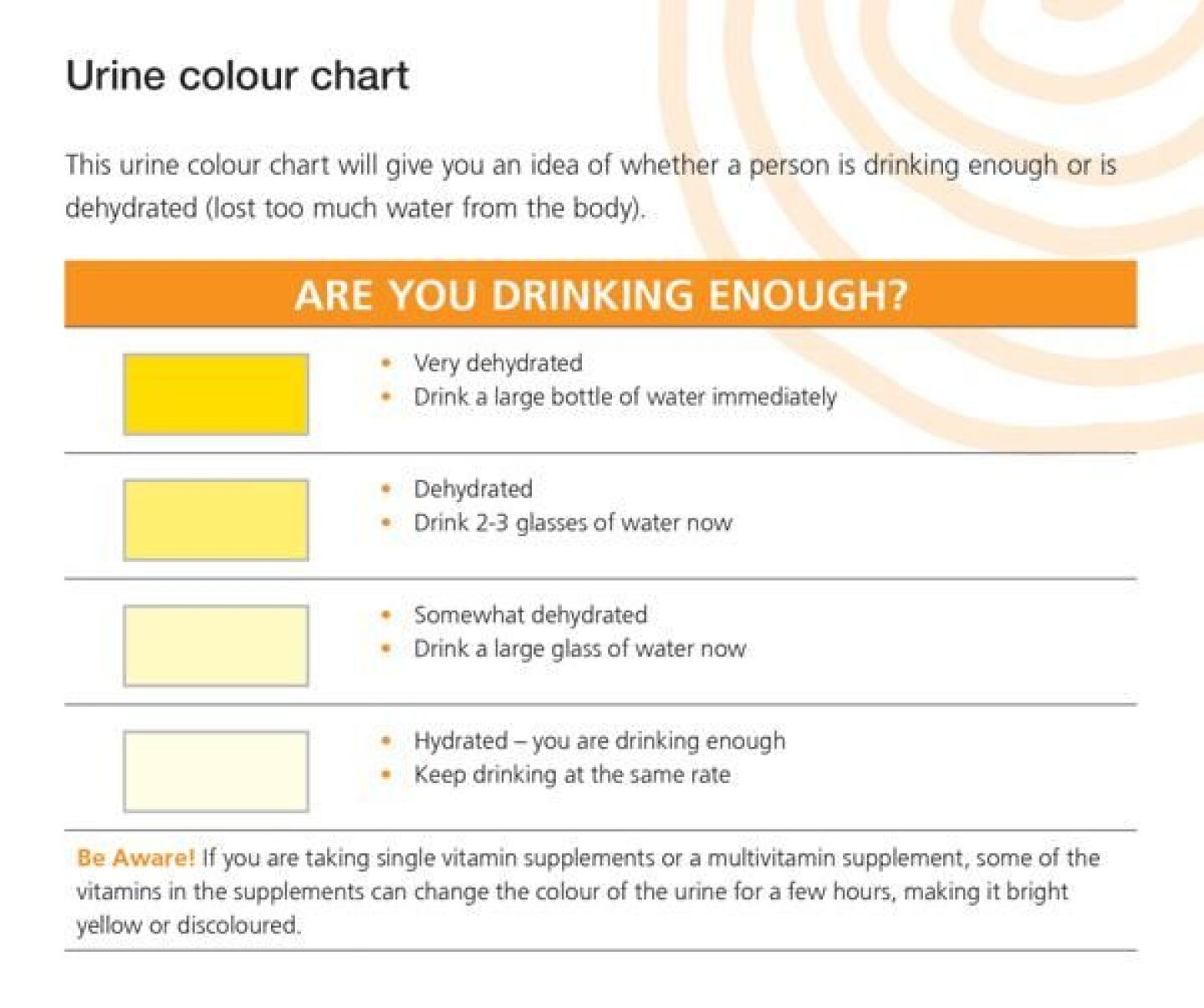
In the summertime or during strenuous work or exercise, we are prone to the combination by forgetting to intake adequate amounts of water and salt while experiencing an increased loss of water and salt through sweating. The kidneys now have less water to work with and must produce more concentrated urine. This accounts for the progressively darker urine as you become more dehydrated. Thus we can color code dehydration via “The Pee Color Chart.”
The Pee Color Chart, Urine Color Chart or Pee Chart has been around the exercise community for some time. Although I am a runner (even if certain unkind observers would describe my movement as a slow jog at best), I was not introduced to the Pee Chart until I began work with the U.S. Forest Service Incident Medical Specialists — EMTs trained to support wildland firefighters.
Obviously, firefighting is hard and hot work and dehydration is a serious problem we would like to avoid. This applies to anyone exposed to weather extremes while performing heavy physical activity. Teaching at-risk individuals to watch for changes in their urine color and responding with appropriate fluid intake is considered “effective dehydration prevention.”
But what fluids are best for hydration?
Water is the mainstay for adequate hydration: females should drink around 70 ounces daily, and males 100 ounces. This accounts for 80% of our daily water requirement; the rest is provided in the foods we eat.
How to use pee color chart
It is often recommended that thirst should guide our liquid intake; however during periods of heavy activity and/or increased environmental temperatures, if you wait until you are thirsty before you drink, you may already be dehydrated.
Using a urine color chart can help. If your urine is clear or very light yellow, you are excreting a normal amount of water which reflects an adequate amount of water in your system. As the color gets progressively darker, that indicates the urine is becoming more concentrated due to a decrease in body water.
A general rule is to use water alone for mild exertion and minimal sweat loss, and then add sports drinks to your water consumption as your exertion and sweating increases. It’s best to avoid drinks containing caffeine or alcohol as they have a diuretic effect and can cause you to lose water. When do we add a “sports drink?” In addition to the water, sports drinks contain varying amounts of salts (sodium, potassium, magnesium, calcium) and one or more carbohydrates (sucrose, glucose, fructose, maltodextrin). Some brands also contain protein.
Over-hydration can cause serious illness
On the reverse side, over-hydration can cause serious problems, such as during past marathon race events where some participants received large amounts of intravenous fluids at the end of the race or military recruits who were required to drink two or more quarts of water per hour during their training day.
Over-hydration dilutes the sodium in the circulation producing a low sodium level (hyponatremia) that can cause serious illness and, on occasion, death. Because of these experiences, athletes and the military have adopted less aggressive fluid replacement practices. However, keep in mind that the majority of problems with body water balance involve dehydration and not over-hydration.
Use a pee color chart to stay hydrated
Although certain abnormal conditions can cause urine to be dark in color — for example, muscle protein (myoglobin) from a crush injury to large muscles or blood (hematuria) from kidney stones or a tumor — in the normal individual, a darkening urine signals a decreasing internal body water content or dehydration.
So, for yourself, watch your urination coloration and stay hydrated. And for your potentially dehydrated patient, add a “U” to your OPQRST and inquire about fluid intake and urination during the “L” — last ins and outs — in SAMPLE.
This article, originally published August 21, 2008, has been updated with current information.
EMS1 is using generative AI to create some content that is edited and fact-checked by our editors.