Presentation #1
| Related Article: Spinal Cord Injury |
You arrive on scene and find a patient who has experienced a traumatic event with a mechanism of injury that you suspect might be enough to produce spinal cord or vertebral injury. You have your partner take manual inline spinal stabilization as you proceed with your initial assessment. You find no immediate life threats and continue with a rapid trauma assessment.
While assessing for neurologic deficits, you note that the patient has no motor (movement) function to the right side of the body. You also note that the patient cannot feel light touch on the right; however, he does complain of pain when you pinch the right hand and foot. As you move to the opposite side of the body, you note that the patient has good motor function and is able to feel light touch on the left hand and foot. However, when you pinch the left hand and foot, the patient doesn’t feel the pain.
These particular assessment findings may appear somewhat confusing to the EMS personnel as the patient exhibits a variation of movement and feeling between the right and left sides. Some EMS practitioners would be deceived into thinking that this is not a spinal cord injury as the patient has some type of neurologic function on both sides of the body. However, similar situations can prove otherwise.
Presentation #2
Looking at another traumatic event, an elderly patient has experienced a mechanism of injury consistent with hyperextension of the neck as a result of an auto crash. Upon your arrival, the patient is out of the vehicle and walking around. During the assessment, you find that the patient has good motor function in the lower extremities, enabling him to walk around; however, the patient has no motor function in both upper extremities when asked to “squeeze my fingers.” Again, these findings would be confusing and inconsistent with a spinal cord injury as the patient has good motor function to the lower portion of the body and no motor function to the upper portion of the body.
Presentation #3
You arrive on the scene and find another trauma patient who received a significant blow to the anterior upper body and neck. During your assessment, you note that the patient has no motor movement and can feel no pain to both sides of the body; however, the patient is able to feel light touch on his hands and feet. Many EMS practitioners would assume that if the patient is able to feel light touch, he would surely be able to feel painful stimuli applied to the body.
In this case, if the EMS personnel made this assumption, they might have never realized that patient was truly unable to feel pain when applied to the body. Once again, the assessment findings are confusing, do not fit the standard definition of a spinal cord injury, and may once again lead to an improper field diagnosis and treatment.
Many EMT textbooks describe a spinal cord injury as presenting with the absence of motor or sensory function below the level of the spinal cord injury. This definition is true when the cord is completely severed, either physiologically or physically, and no nerve impulse transmission occurs above or below the level of injury. None of the aforementioned patient presentations fit this standard definition; however, these assessment findings are consistent with incomplete spinal cord injury. One must wonder if EMS personnel would fail to recognize the conflicting assessment findings as evidence of an incomplete spinal cord injury, misdiagnose the condition, and improperly treat the patient.
The Spinal Cord
The spinal cord is comprised of central nervous system tissue and requires a constant supply of oxygen and glucose. One anterior spinal artery and two posterior spinal arteries deliver blood to the cord. The anterior artery supplies approximately two-thirds of the anterior and middle section of the cord while the posterior artery provides the remaining one-third of the posterior cord with blood. Injury to these arteries may produce nerve cell ischemia and result in neurologic dysfunction.
The cord is separated into right and left halves by the anterior medial fissure and posterior medial sulcus. The central portion of the cord contains gray matter that is comprised of cell bodies of neurons and forms an “H” pattern. The surrounding white matter contains motor and sensory nerve tracts. The motor tracts transmit nerve impulses from the brain, down the spinal cord, and to the efferent nerve tracts to muscles that produce movement. The sensory tracts transmit impulses such as pain, pressure, heat and light touch from afferent nerve tracts up the cord to the brain where the information is processed.
The corticospinal tracts are responsible for motor nerve transmission and control movement. These tracts are located in the lateral aspects of the cord. The impulse traveling down the right corticospinal tracts control movement on the right side of the body. Thus, an injury to the left corticospinal tract will produce motor dysfunction on the left side of the body; however, the patient will retain motor function on the right.
The posterior columns (fasciculus gracilis and fasciculus cutaneous) are located in the posterior portion of the spinal cord and carry sensations of position (proprioception), vibration, and light touch from the skin, muscles, tendons, and joints to the brain. The sensation impulses are carried up the same side of the cord where the stimulus is applied. If the left hand is touched, the sensory impulse is carried up the posterior columns on the left side of the body. If an injury were to occur to the left posterior columns, the patient would retain the ability to feel light touch on the right side of the body.
The spinothalamic tracts carry the sensations of pain, temperature, pressure and crude touch to the brain. Interestingly, these nerve tracts crossover to the opposite side shortly after entering the spinal cord. Thus, pain applied to the right side of the body is actually carried up the left spinothalamic tract on the left side of the spinal cord. An injury to the left spinothalamic tract would result in the patient losing the ability to feel pain to the right side of the body.
Uncovering Incomplete Spinal Cord Injury
Based on the understanding of what impulses are carried by the different spinal tracts and where the tracts are located within the spinal cord, one can begin to explain the three incomplete spinal cord injury presentations at the beginning of this column.
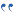 The key in your assessment of these conditions is realizing that the spinal cord is only partially injured. The key in your assessment of these conditions is realizing that the spinal cord is only partially injured.  |
The first traumatic event described is a Brown-Sequard syndrome where the right hemisection of the cord is injured. The left hemisection remains intact and functional (the opposite findings would occur if the left hemisection was injured). Motor function and light touch are lost on the side of the cord injury because the motor and light touch tracts carry the impulses on the same side of the body; however, the pain sensation is preserved because the impulse is carried on the opposite side of the cord that is not injured. Take note, though, that the pain sensation was lost on the left side where motor function and light touch was functional. This occurred due to the interruption of the right spinothalamic tract that carries the sensation of pain from the left side of the body up the opposite (right, in this case) side of the spinal cord.
The second traumatic event described is a central cord syndrome. The central portion of the cord is injured while the lateral aspect remains intact. The upper extremities are controlled by nerve tracts found in the medical aspect (inner portion) of the corticospinal tract; whereas, the legs are controlled by nerve tracts in the lateral (outer portion) of the same corticospinal tract. Thus, an injury to the medial aspect of both corticospinal tracts — which occurs in a central cord syndrome — results in loss of motor function to the upper extremities, while the outer portion of the tract is unaffected and motor function is preserved in the lower extremities. The same finding may occur with the spinothalamic tracts. The patient loses the sensation of pain in the upper extremities but maintains the ability to sense pain in the lower extremities. This is common in patients with degenerative arthritis where a hyperextension injury drives the ligamentum flavum into the central portion of the spinal cord causing injury to the medial (inner) portions of the various tracts.
In the third traumatic event, the anterior vertebral artery has been injured and the anterior portion of the spinal cord has lost adequate perfusion resulting in ischemia and neurologic deficit. Because the spinothalamic tracts are located in the anterior portion of the cord, the patient loses the ability to sense pain on both sides of the body. If the injury extends farther into the cord, the patient’s motor ability might also be affected.
Conclusion
The key in your assessment of these conditions is realizing that the spinal cord is only partially injured; thus, only certain tracts are affected, resulting in specific neurologic deficits and not a complete loss of motor and sensory function below the level of injury. Any patient who presents with any loss of sensation of pain or light touch or motor function, whom has experienced a mechanism that may produce a spinal injury, should be suspected of having an incomplete spinal cord injury. Although these conditions may provide conflicting and confusing assessment findings, it is extremely important to understand that the spinal cord is indeed injured and that the patient requires complete spinal immobilization.


