My first intraosseous happened during my paramedic training in the mid-1990s. My preceptor talked me through inserting an 18-gauge Jamshidi into the proximal tibia of a three-month-old child thrust onto the kitchen table in front of me. I used the IO needle just as I was instructed — on a baby in cardiac arrest after two unsuccessful IV attempts.
Like many paramedics, my original view of an IO insertion was that it was a stressful, high-risk, low-frequency skill performed as a last resort. Fortunately, my view of this skill has changed dramatically during my career as a flight paramedic and member of a specialty pediatric transport team.
Caring for a sick child is stressful enough, but there is little that matches the feeling of hopelessness that comes with being unable to provide drugs or fluids because I can’t get an IV. So in the interest of relieving some stress when you find yourself with a sick child and no IV access in a similar situation, consider the following five tips to improve your comfort and confidence with IO insertion and maintenance.
1. Just do it.
New technology is making IO insertion easier and available to more patients than ever [1]. Both Pediatric Advanced Life Support and Advanced Cardiac Life Support guidelines have removed endotracheal drug administration in favor of IO routes, making the skill acceptable in almost any age of patient.
As well as its traditional role as rescue access, IO access can also be considered as a secondary access source if the initial line is questionable, it is too small or the patient requires large volumes of fluid, vasopressors or other drugs that may irritate the vasculature. Non-emergent IO access has been discussed in the anesthesia literature, reporting semi-elective use in the operating room [2]. The relatively minimal insertion pain with newer devices begs the question — is it better for the patient to have a single IO inserted or multiple unsuccessful IV attempts?
Technology and experience have overcome all of my original reluctance. The IO is no longer just my Hail Mary access in cardiac arrest. I now consider it on any patient without vascular access if a delay in fluid or drugs could be harmful.
2. Have a back-up plan.
In my experience, the proximal tibial tuberosity is probably the most recognized site for insertion, but there are several reasons that this site may be inappropriate. Some of these reasons include: burns, orthopedic trauma, local infection, previous IO attempts or inability to access in a trapped patient.
Remember, a number of alternative sites exist. Animal models suggest that humeral and femoral flow rates are higher compared to the proximal tibia [3]. However, first attempt insertion success was lower (89% vs. 60%) and the risk of dislodgement was higher (33% vs. 6 %), when the humeral site was compared with the proximal tibia [4]. The sternum, iliac crest, distal tibia, calcaneus, radius and ulna have also been attempted with varying degrees of success and complication rates [5].
I now have a back-up plan in the event the proximal tibia is unavailable. In older children — typically kids over six years old, but the child’s size is more important than age — my alternative site is the proximal humerus, as the distal femur can be challenging because of the deeper layers of muscle and tissue. In children under the age of six, my alternative site is the distal femur, as it is easier to access and avoids the difficulties associated with an anatomically small humerus.
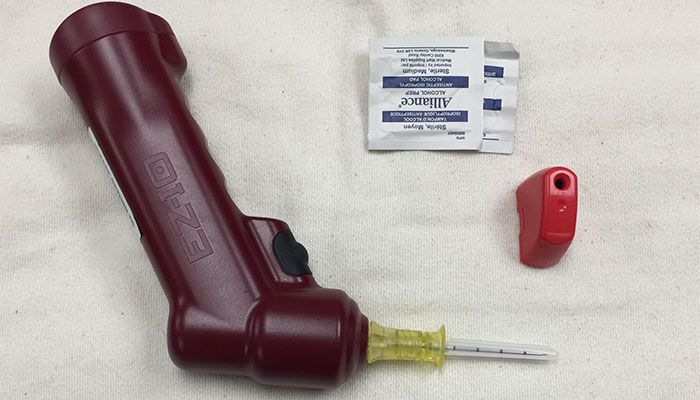
3. Confirm Pediatric IO Placement
Traditional techniques such as palpating the posterior limb for signs of infiltration during a saline flush, as well as noting the stability of the needle after insertion, are familiar methods of confirming placement. The aspiration of blood from the needle confirms placement, however it is important to remember that the absence of blood does not necessarily mean the IO is interstitial.
A new technique for confirming placement has recently been added to my practice. It is based on animal studies that demonstrated that when soft tissue around the needle is compressed with two hands for 10 seconds, the pressure within the IV line increases if the device is interstitial [6]. Squeezing the soft tissue should have no effect on flow rate if the catheter is in the medullary space. Practically speaking, if the flow rate of the IO stops while squeezing the soft tissue, the IO is likely interstitial.
4. Plan for pain and anxiety.
Broadening the IO insertion criteria produces new challenges. Now that the patient may be conscious, it presents two new problems: pain and anxiety.
Pain surrounding IO insertion is lower than pain associated with infusion and is generally well tolerated [7]. Pain requiring treatment may occur with infusions, especially with higher flow rates. First-line treatment for this pain is instilling 2% lidocaine (0.5 mg/kg < 39 kg or 20-40 mg > 40 kg) into the IO, followed by a 10 mL saline flush; ideally 30 seconds prior to beginning any infusion [5]. Repeat dosing may be required. If the pain persists, narcotic administration may become necessary.
Anxiety can almost always be lessened with good communication, so explaining the procedure to both parents and child is imperative. Anxious parents lead to anxious children and a few moments of thoughtful explanation can pay dividends before a mother sees you holding a cordless drill and their sick child’s leg all at the same time.
5. Know what to watch for.
Severe complications are rare, but do occur and many are preventable. Dislodgement is the most common complication of IO infusions. Trauma to the bone, including fractures, and soft tissue is also possible. Infectious side effects can range from local abscess to osteomyelitis or septicemia [8].
The following are part of my routine for inserting and managing IO infusions: be clean, be gentle and pay attention. First, the skill is invasive and should be performed in an aseptic manner. Second, while it is important that the device is secured, be cautious of roller gauze and tape that prevents ongoing assessment of distal circulation and may obscure signs of extravasation or poor distal perfusion. Finally, be mindful of not forcefully pushing drugs and fluid as it may dislodge the needle. Extravasation can lead to soft tissue necrosis, compartment syndrome or even amputation [9]. Remember, an IO should never be left unmonitored.
I am thankful that over the years my view of intraosseous access has changed. It used to represent everything that was terrifying about pediatrics: tiny veins too sick to cannulate, forcing me to perform a procedure of last resort — something I was sure would prevent the child from ever walking properly. A combination of new equipment and experience has changed my opinion and intraosseous access has become my security blanket. I know that regardless of what the vein looks like I will be able to obtain access. Provided I am careful, the benefits of inserting an IO far outweigh the risks.
This article, originally published August 23, 2016, has been updated
References
- Myers, L.A., Russie, C.S., & Artega, G.M. (2011). Semiautomatic Intraosseous devices in pediatric prehospital care. Prehospital Emergency Care, 15:473-476
- Neuhaus, D., Weiss, M., Engelhardt, T., Henze, G., Giest, J., Strauss, J., & Eich, C. (2010). Semi-elective intraosseous infusion after failed intravenous access in pediatric anesthesia. Pediatric Anesthesia, 20: 165-171
- Lairet, J., Bebarta, V., Lairet, K., Kacprowicz, R., Lawler, C., Pitotti, R., Busch, A., & King, J. (2013). A comparison of proximal tibia, distal femur and proximal humerus infusion rates using the EZ-IO intraosseous device on the adult swine model. Prehospital Emergency Care, 17:280-284
- Reades, R., Studnek, J.R., Garret, J.S., Vandeventer, S., & Blackwell, T. (2011). Comparison of first-attempt success between tibial and humeral intraosseous insertions during out-of-hospital cardiac arrest. Prehospital Emergency Care, 15:278-281
- Paxton, J.H. Intraosseous vascular access: A review. (2012). Trauma, 14(3): 195-232
- Lee, B.K., Jeung, K.W., Lee, H.Y., Lee, S.J., Bae, S.J., Lim, Y.D., Moon, K.S., Heo, T., & Min, Y.I. (2014). Confirmation of intraosseous cannula placement based on pressure measured at the cannula during squeezing the extremity in a piglet model. Resusciation, 85:143-147
- Fowler, R.L, Pierce, A., Nazeer, S., Philbeck, T.E., & Miller L.J. (2008) 1,199 Case Series:Powered intraosseous insertion provides safe and effective vascular access for emergency patients. Annals of Emergency Medicine, 52(4) S152
- Cullen, P.M, (2011) Intraosseous cannulation in children. Anaesthesia and Intensive Care Medicine, 13(1): 28-30
- Suominen, P.K., Nurmi, E., & Lauerma, K. (2015) Intraosseous acces in neonates and infants: risk of severe complication – a care report. Acta Anaesthesiologica Scandinavica, 59: 1389-1393
References reviewed
- Distal Femur Site Identification & Insertion Technique (Infant/Child) (nd) Retrieved from: http://www.teleflex.com/en/usa/ezioeducation/index.html
- Proximal Humerus Site Identification & Insertion Technique (Infant/Child) (nd) Retrieved from: http://www.teleflex.com/en/usa/ezioeducation/index.html




