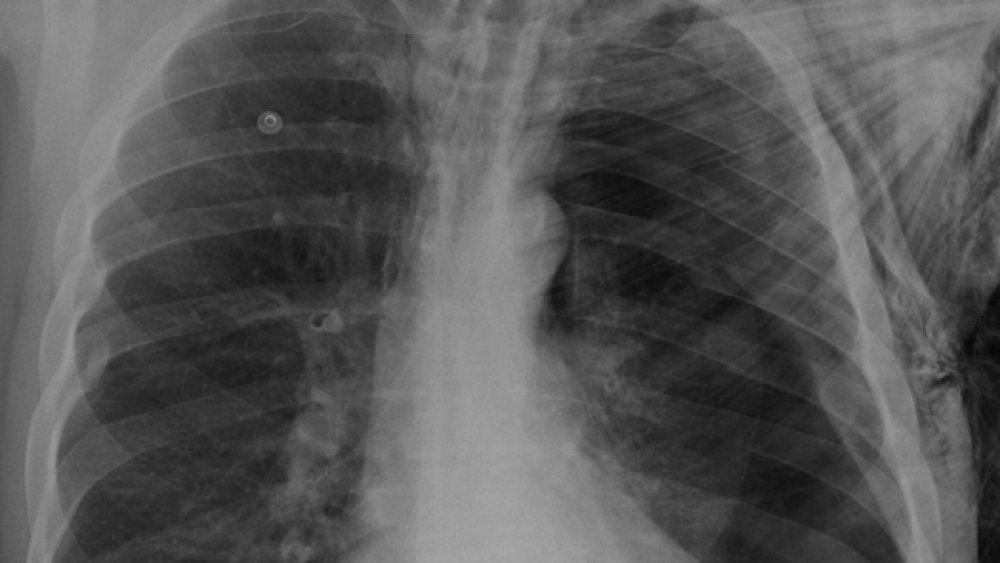
Tension pneumothorax is a condition that can quickly cause death from respiratory and circulatory compromise [1]. Prompt recognition of tension pneumothorax and treatment with needle decompression can be lifesaving [1-3].
However, it is also important to differentiate tension pneumothorax from conditions with similar symptoms, and to avoid performing inappropriate needle decompression. Waveform capnography and ultrasound are two tools that EMS providers can use to help identify tension pneumothorax and determine if treatment is effective.
Tension pneumothorax overview
A pneumothorax is a condition where damage to lung tissue causes air to leak into the pleural space. The pleural space is normally a potential space with a small amount of fluid lining the lungs and chest wall. With a pneumothorax, pressure changes in the chest can cause more air to enter the pleural space during inhalation, which creates a one-way valve that traps air in the pleural space on exhalation. This progressive increase in pressure can cause the lung to collapse leading to respiratory compromise.
A tension pneumothorax occurs when pressure in the pleural space is so high that it compresses the heart and great vessels, in addition to the lungs [1]. Pressure on the vena cava reduces blood flow to the heart and impairs cardiac output, leading to respiratory and circulatory compromise. A pneumothorax can evolve into a tension pneumothorax rapidly, or develop during the course of care.
A pneumothorax can be caused by blunt or penetrating chest trauma, positive pressure ventilation, or can occur spontaneously. Signs and symptoms of a pneumothorax include difficulty breathing, chest pain that is usually sharp and increases with inhalation, decreased or absent breath sounds on the affected side, and subcutaneous emphysema.
A tension pneumothorax also has signs of poor perfusion, such as agitation, altered mental status, tachycardia, hypotension. Jugular venous distention and tracheal deviation are late and unreliable findings of tension pneumothorax [1,2].
For patients receiving positive pressure ventilation, consider a pneumothorax if there is a high-pressure alarm on the ventilator or if it is difficult to squeeze a bag-valve mask.
Administer high flow oxygen for any pneumothorax. Perform needle chest decompression for a tension pneumothorax.
A pneumothorax of any size can affect oxygenation and ventilation. Pulse oximetry and capnography should be monitored in any patient with a suspected pneumothorax, and high-flow oxygen should be administered via non-rebreather mask. Avoid assisted ventilation with a bag-valve mask if at all possible – unless respiratory arrest is imminent, because positive pressure can worsen a pneumothorax [1,2].
Read more ...
Tension Pneumothorax: Identification and treatment
Tension pneumothorax is a life threatening condition that can occur with chest trauma and is more likely to happen with trauma involving an opening in the chest wall
Definitive treatment for a pneumothorax is a chest tube, though a small pneumothorax may resolve on its own. In most trauma systems chest tubes are placed in the hospital and not by EMS.
For a tension pneumothorax, where there are signs of respiratory failure and hypoperfusion, a needle chest decompression is a temporizing measure to relieve pressure in the chest until a chest tube can be placed. PHTLS recommends needle chest decompression should be done for patients with:
- Worsening shortness of breath or difficulty with assisted ventilation
- Decreased or absent breath sounds on one side
- Blood pressure less than 90 systolic with narrow pulse pressure [2]
This paramedic-level skill involves placing a large-bore needle and a 16-gauge or larger catheter, in the second intercostal space at the midclavicular line, just above the third rib. Chest wall thickness can vary, and there is a significant rate of failure from needles not penetrating the chest wall [1].
PHTLS recommends using a needle that is at least 8 cm (3.5 inches) long; using the standard 5 cm needle and intravenous catheter will not penetrate the chest wall up to 42 percent of the time [2]. Insert the needle until a rush of air is felt, remove the needle, and leave the catheter in place. Vital signs and ventilation should rapidly improve if successful.
Only a tension pneumothorax should receive needle decompression, and the procedure carries a number of complications when performed when it is not indicated [4]. In addition to causing significant pain, it will cause a small pneumothorax if the needle penetrates the lungs. There is also risk of damage to nerves and blood vessels that are under the ribs. Even when pneumothorax is indicated and an 8 cm needle/catheter is used, there is a chance that the needle will not penetrate the chest wall.
The role of capnography in tension pneumothorax
It is important to be judicious with patient selection for needle decompression, and to determine whether or not it worked. Here is how waveform capnography and ultrasound can help.
Waveform capnography provides continuous feedback on ventilation and perfusion. Through a sample of exhaled air captured from nasal prongs, or an adaptor connected to a bag-valve mask or advanced airway device, each exhalation generates a rectangular-shaped waveform on the capnograph. Capnography also measures the amount of carbon dioxide exhaled with each breath (ETCO2), which is normally 35-45 mm Hg.
When ventilation is compromised, such as with a pneumothorax, CO2 cannot be eliminated effectively and it builds up in the lungs. This causes a higher concentration of CO2 to be exhaled with each breath, and for ETCO2 to rise. In the setting of a suspected pneumothorax, a high or increasing ETCO2 (above 45 mm Hg) suggests that it is getting worse.
ETCO2 is also affected by perfusion to the lungs. With a tension pneumothorax, decreased cardiac output causes less CO2 to be delivered to the lungs for exhalation. This would cause ETCO2 to be low – below 35 mm Hg. Thus, as a pneumothorax evolves, ETCO2 would first increase due to inadequate ventilation, and then decrease when circulation is impaired from a tension pneumothorax. A normal to high ETCO2 effectively rules out a tension pneumothorax and the need for needle decompression, and a decrease in ETCO2 may be the first sign of a tension pneumothorax.
When needle chest decompression is performed, ETCO2 is one of the first vital signs to change if it is successful. As air is released from the pleural space, ETCO2 will rapidly increase. If there is no change in ETCO2 after decompression, assess whether the needle penetrated the chest wall, and reassess whether a tension pneumothorax was present in the first place.
In patients with chest injuries or receiving assisted ventilation, however, changes in ETCO2 are not specific to a pneumothorax. Pain from rib fractures on inhalation may cause patients to hypoventilate and for ETCO2 to increase. Hypovolemic shock and traumatic arrest also cause low ETCO2 from decreased perfusion.
Waveform capnography is the gold standard to confirm airway placement in intubated patients. In addition to pneumothorax, ET tube dislodgement, obstruction, and equipment failure are other possible causes of ETCO2 loss. A right mainstem intubation will also cause a decrease in ETCO2, along with decreased breath sounds on the left side. Reassess tube placement, patency, and depth in intubated patients before treating for a tension pneumothorax.
The role of ultrasound for tension pneumothorax
Ultrasound is emerging as a tool for EMS to identify a number of conditions, and is highly sensitive and specific to diagnose a pneumothorax. When examining a normal chest with ultrasound, movement of the lung along the chest wall can be seen with a characteristic sliding lung sign during the respiratory cycle. The sliding motion disappears from air in the pleural space from a pneumothorax [5].
Ultrasound has also been used in the military to triage patients with a suspected pneumothorax, and has helped prevent unnecessary needle chest decompression, chest tubes, and transfer to higher levels of care [6]. In another study of 57 patients who received needle decompression by paramedics, 26 percent were found to have no pneumothorax when assessed by ultrasound in the emergency department, and it was determined that no chest tube was needed [7].
There is also evidence suggesting a short learning curve for ultrasound. A study of 20 paramedics showed that after a two-hour training session on ultrasound, paramedics could correctly identify pneumothorax, pericardial effusion, and cardiac activity [8].
Ultrasound would be especially useful to detect pneumothorax in situations when a physical exam and lung sound assessment are difficult, such as a helicopter transport. Look for this technology to become more widely available in the near future.
Tension pneumothorax is a critical diagnosis for EMS providers to make, and to differentiate from conditions with similar signs and symptoms. Waveform capnography and ultrasound are two tools that can improve diagnostic accuracy of tension pneumothorax.
This article was originally posted May 12, 2016. It has been updated.
References
1. Page D, Chu S, Bown M, Lyman K. Tension Pneumothorax. EMS Reference (2015) Retrieved from: https://emsreference.com/articles/article/tension-pneumothorax-0
2. Prehospital Trauma Life Support Committee of the National Association of Emergency Medical Technicians in cooperation with the Committee on Trauma of the American College of Surgeons. PHTLS: Prehospital Trauma Life Support. 8th ed. Burlington, MA: Jones and Bartlett
3. Weichenthal L, Crane D, Rond L. (2016): Needle Thoracostomy in the Prehospital Setting: A Retrospective Observational Study, Prehospital Emergency Care [Epub ahead of print] DOI:10.3109/10903127.2015.1102992
4. Warner K, Copass M, Bulger E. (2008). Paramedic Use of Needle Thoracostomy in the Prehospital Environment. Prehospital Emergency Care, 12 (2): 162-168.
5. Sun J, Juang C, Huang Y, Sim S, Chong K, Wang H, Lein W. (2014). Prehospital Ultrasound. Journal of Medical Ultrasound; 22:71-77.
6. Roberts J, McManus J, Harrison B. (2006). Use of Ultrasonography to Avoid an Unnecessary Procedure in the Prehospital Combat Environment: a Case Report. Prehospital Emergency Care; 10:502-506
7. Blaivas M. (2010). Inadequate Needle Thoracostomy Rate in the Prehospital Setting for Presumed Pneumothorax. Journal of Ultrasound in Medicine; 29 (9): 1285-1289
8. Chin E, Chan C, Mortazavi R, Anderson C, Kahn C, Summers S, Fox J. (2013). A Pilot Study Examining the Viability of a Prehospital Assessment with UltraSound for Emergencies Protocol. Journal of Emergency Medicine; 44 (1): 142-149.